Viruses are microorganisms that cause common infectious diseases such as cold and flu and many severe illnesses. Although tiny, viruses invade healthy cells in a body and use them to multiply and produce other viruses like themselves.
Not all viruses are the same and they usually attack different types of cells. Throughout this post, we’re going to discuss human papillomavirus. Scroll down to learn about its types, causes, symptoms, treatment options, and more.
Overview of Human Papillomavirus (HPV)
Human papillomavirus (HPV) is a viral infection that is transmitted from one person to another through skin-to-skin contact. The virus got its name because many strains cause warts which are known as papillomas.
Records show that the virus was first discovered[1] in 1956 by a group of scientists. The interest in the HPV increased significantly after 1984 when a German virologist and professor Harald zur Hausen discovered, cloned, and attributed cervical cancer to HPV 16 and 18.
You see, HPV is not a single virus, there are more than 100 varieties, 40 of which are passed through sexual contact. Not all types of HPV are equal.
While some varieties cause genital warts others can contribute to different types of cancer. Below, we’re going to discuss types, causes, and other important details about this common virus.
How Common is HPV?

According to the Centers for Disease Control and Prevention[2] (CDC), about 79 million Americans are currently infected with HPV and 14 million people become newly infected each year.
In fact, the virus is so common that every sexually active man or woman will get it at some point in their lives unless they don’t get an HPV vaccine. This means that HPV is the most common sexually transmitted infection (STI) in the United States.
In 2013-2014, the prevalence of genital infection with any HPV type was 42.5% among adults aged 18-59 years. Despite a decline in the prevalence[3] of vaccine-type HPV infection and genital warts, the overall infection rates are still unacceptably high.
High-risk genital HPV infection affects 25% of men and 20% of women while the prevalence of oral infection (any type) was 7% and high-risk oral infection 4% among adults.
Figures show[4] that each year 39,800 new cases of cancer are found in parts of the money where HPV is often found. The human papillomavirus causes about 31,500 of these cancers.
What are The Common Types of HPV?
As stated above, more than 100 types of HPV have been identified so far. Not every strain is equal, some are high-risk while others low-risk types.
Low-risk human papillomavirus types include HPV 6 and 11 and a number of less common variants. The term low-risk HPV indicates that some particular type is non-oncogenic i.e. it doesn’t cause cancer.
In most cases, these strains cause genital warts. Infections with these types rarely increase the risk of cervical or some other cancer. The HPV 6 and 11 cause[5] about 90% of all genital warts cases.
They tend to resemble bumps or cauliflower and usually show up weeks after sexual intercourse with a partner.
On the other hand, high-risk HPV is also called oncogenic due to its ability to cause cervical cancer and increase the risk other serious illnesses such as penile, anal, and throat cancer.
Although high-risk HPV types are oncogenic, it doesn’t mean every man or a woman who is infected with these strains will develop cancer for sure. Common high-risk human papillomavirus types include: HPV 16, 18, 31, 33, 35, 45, 52, 58, and 59.
The HPV 16 and 18 account for[6] about 66% of cervical cancers in the US, 25% of low-grade, and 50% of high-grade of cervical intraepithelial lesions or dysplasia.
Also, these types of HPV cause about 79% of cases of anal cancer. Approximately 8% anal cancers are caused by HPV 31, 33, 45, 52, and 58.
How Does Human Papillomavirus Spread Though the Body?
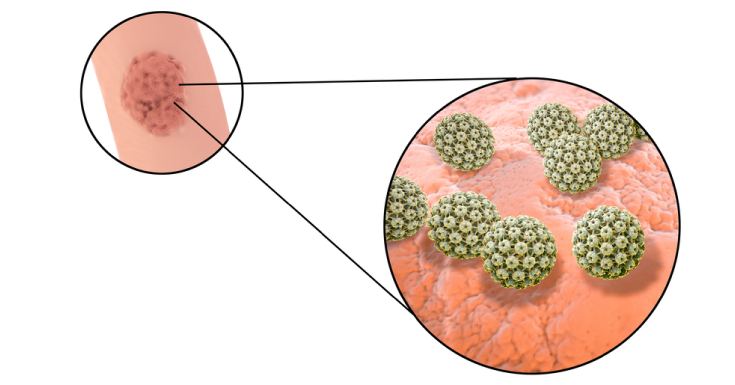
The human papillomavirus is very common, but how does it infect people? The infection occurs when the virus enters a person’s body. The virus reaches your body through a cut, small tear in the skin, or abrasion. The HPV is transmitted primarily through a skin-to-skin contact.
The skin-to-skin contact is usually through oral, anal, and vaginal sex. The virus can be passed from one person to another even when an infected individual has no signs and symptoms of infection.
The severity of this virus is best depicted by the fact that infants can get it during birth. If a pregnant woman has an HPV infection with genital warts, these warts may enlarge and multiply during pregnancy.
In this case, treatment has to wait until an infected woman gives birth to her baby and increases the risk of infecting the baby.
Warts are considered contagious. It’s easy to spread them through direct contact with the wart or by touching something that was in contact with them.
What are The Risk factors of HPV Infection?
All sexually active men and women can get HPV, but some factors increase the risk significantly. Common risk factors include:
- Age – Children are more likely to develop common warts while teenagers and young adults usually develop genital warts
- Contact With Warts – Common warts are contagious and one can get infected easily. Your risk of HPV infection increases when you touch someone’s warts or if you come into contact with a surface that has been exposed to the virus e.g. publish showers and swimming pools.Since children usually develop common warts they are likely to get infected in this manner
- Damaged Skin – Common warts are more likely to develop on areas of skin that are damaged by cuts or abrasions i.e. having any sort of wound or opening on the skin’s surface increases the risk of getting common warts
- A Number of Sexual Partners – Due to the fact that HPV transmits from one person to another and usually through sexual intercourse the number of sexual partners plays a role in the risk of getting the infection too.
The more sexual partners you have, the more likely you are to get HPV. Also, the number of sexual partners that your significant other has had matters too. The more sexual partners they had, the greater the odds of getting HPV - Weak Immune System – Having a weaker immune system puts you at risk of developing the virus because the immunity isn’t strong enough to put up a good defense. This is particularly the case in persons with HIV and patients who have undergone an organ transplant

What are The Symptoms of HPV Infection?
It’s not uncommon for a person to have HPV without experiencing any symptom whatsoever. In many cases, the immune system fights off the infection before it gets the chance to cause the formation of warts. When they do form, warts vary in shapes, sizes, and locations depending on the type of virus.
Below, you can see the types of warts associated with HPV:
Common Warts – Rough, raised bumps that develop mainly on the fingers, hands, and elbows. These warts aren’t dangerous but can be prone to bleeding, injury, and an affected person can find them painful too
Flat Warts – Slightly raised, flat-topped lesions that are slightly darker than your natural complexion. Men, women, and children can develop them, but in different places. Men develop flat warts in beard area, women on legs, and children on their face
Genital Warts – Flat lesions that look like a cauliflower. In women, genital warts develop on the vulva (the external part of female genitalia), but they can also form near the anus, cervix (lower part of the uterus, connects it with a vagina) and in the vagina.
Contrary to the popular belief, men can develop genital warts too. Male patients develop these warts on the penis, scrotum, and near the anus. Although genital warts rarely cause pain and discomfort, they can be itchy.
HPV viruses that cause genital warts aren’t the same as the ones that cause cancer. This means that if you have warts in genital area, it doesn’t automatically indicate you’ll develop a serious disease too
Plantar Warts – Grainy, hard growths that are primarily located on balls and heels of the feet and can be very uncomfortable
Signs of an infection can appear days, weeks, months, and even years after a patient has been infected by the HPV virus.
How Cancer is Linked to HPV?
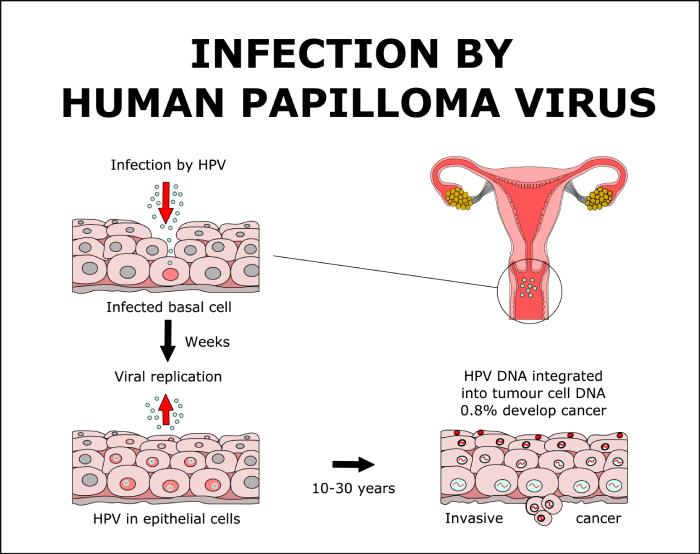
High-risk types of HPV are closely associated with different types of cancer. If a person gets infected with one of the above-mentioned high-risk HPV types, it is possible to develop precancerous changes in cells in the tissue without any symptoms.
The relationship between high-risk HPV and cancer is so strong that you’ll usually find multiple resources discussing it in the same section as symptoms of HPV. Below, you can see the basic rundown of the different types of cancer associated with this virus.
Cervical Cancer
Cervical cancer was briefly mentioned above and it’s not uncommon for people to think that it’s the only type of cancer one can get from HPV. Cervical cancer is a serious disease that occurs in cells of the cervix.
How Does HPV Cause this Disease?
When a woman is exposed to genital HPV, her immunity usually prevents the virus from causing any harm. That said, in some women, the virus survives for years and converts normal cells on the surface of the cervix into cancerous cells.
At the very beginning, the growth of cancerous cells may manifest itself as a viral infection, but later precancerous changes occur.
According to the American Cancer Society[7], about 13,240 new cases of invasive cervical cancer will be diagnosed in 2019 in American women and about 4170 women will die due to this severe disease.
The primary cause of this cancer is HPV and it is most frequently diagnosed in women between the ages of 35 and 44. The incidence of cervical cancer among women who are younger than 20 is very rare.
Symptoms of cervical cancer include pelvic pain and pain during sexual intercourse, vaginal bleeding after intercourse (between periods or after menopause), and watery, bloody vaginal discharge with a foul odor.
Vulvar Cancer
Vulvar cancer is a type of cancer that affects vulva. It usually forms as a lump or sore on the vulva and causes itching. Although women of all ages can develop vulvar cancer, the disease is most commonly diagnosed in older adults.
Estimates show[8] that about 6190 new cases of vulvar cancer will be diagnosed in 2019 and 1200 US women will die due to this disease.
Vulvar cancer is less common than cervical cancer. Symptoms associated with this disease include persistent itching, pain and tenderness, bleeding that is unrelated to menstruation, a lump in the vulva, and a color change or thickening of the affected area.
Just like with cervical and other cancers, HPV can make healthy cells become cancerous and, thereby, contribute to the development of this disease.
Vaginal Cancer
Vaginal cancer is a rare type of cancer that affects the vagina, the muscular tube that connects uterus with outer genitals. The disease develops in the cells that line the surface of a vagina i.e. a birth canal.
According to some estimates[9], about 5170 new cases of vaginal cancer will be diagnosed in 2019 among US women and 1330 ladies will die of this cancer.
Many vaginal pre-cancers contain HPV and these changes may be present for years before they turn into cancer. Symptoms of vaginal cancer include constipation, pelvic pain, watery vaginal discharge, unusual vaginal bleeding, a lump or mass in vagina, painful and frequent urination. The disease usually affects women older than 60.
Penile Cancer
Penile cancer is a type of cancer that develops in or on the penis. Statistics show[10] that 2320 cases of penis cancer will be diagnosed in US men in 2019 and 380 men will die of this cancer.
In North America and Europe, penis cancer is rare and primarily affects men who are older than 60. Symptoms associated with penile cancer include a lump on the penis as well as soreness, redness, and irritation.
Anal Cancer
Anal cancer is a type of cancer that develops in the anal canal and it’s considered uncommon. The anal canal is a short tube at the end of the rectum through which the stool leaves your body.
Figures reveal[11] that in 2019 about 8580 (5620 in women and 2960 in men) new cases of anal cancer will be diagnosed and 1160 deaths (680 in women and 480 in men).
HPV can cause anal cancer in both men and women, but it is more common in people with HIV and men who have sexual intercourse with other men. Signs and symptoms of anal cancer include anal itching, bleeding from anus or rectum, a mass or growth in the anal canal, and pain in the anal area.
Oral Cavity and Oropharyngeal Cancer
Besides cancer in the genital area, HPV can cause mouth (oral cavity) and throat (oropharyngeal) cancer too. The mouth cancer can affect lips, the lining of the lips and cheeks, teeth, gums, the front two-thirds of the tongue, the floor of the mouth below the tongue, and the hard palate.
Most cancers found in the back of the throat, including the base of tongue and tonsils, are HPV-related. Numbers show[12] that about 51,540 people will get mouth or throat cancer in 2019 and about 10,030 people will die of these cancers.
How to Diagnose HPV?
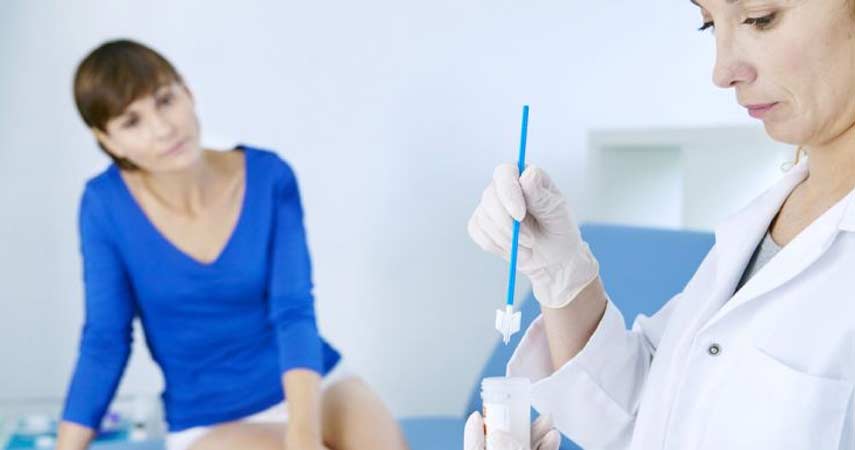
If you have warts chances are high you are infected with HPV, but you should still see your doctor who will make an accurate diagnosis.
Just by looking at your warts the physician will presume HPV is the underlying cause. In some cases genital warts aren’t visible, the doctor may recommend tests such as:
- DNA Test – Carried out on cells from the cervix. This test can recognize the DNA of high-risk HPV types that are associated with cancer in this area. DNA test is recommended for women older than 30 as an addition to Pap test
- Pap Test – a physician collects a sample from vagina or cervix and sends for a laboratory analysis. The purpose of this test is to identify abnormalities that could lead to cancer
- Acetic Acid Or Vinegar Solution Test – The solution is applied to the genital area and makes the infected areas turn white. This test helps doctors spot flat lesions that are difficult to notice otherwise
What is The Treatment for HPV?
Some people can have HPV for years before warts appear and in most cases, they come and go on their own, without any treatment, especially in children.
It’s important to mention that although warts come and go, the virus remains in the body. At this point, there is no cure for HPV.
After the HPV diagnosis, the doctor determines whether you need a treatment or don’t. The doctor recommends an adequate treatment in instances when warts don’t go away on their own. Treatment options revolve around medications and various procedures.
Medications for the treatment of warts are usually topical and it’s important to be patient. You’ll need to apply them regularly in order to eliminate warts. Most common medications used for this purpose are:
- Salicylic Acid – Available as an over-the-counter (OTC) and works by removing layers of warts one after another. However, it can cause irritations in persons with common warts and should not be applied to the face
- Trichloroacetic Acid – Burns off warts on the palms, genitals, and soles. The treatment might cause localized inflammation
- Podofilox (Condylox) – Destroys genital wart tissue, it might cause pain and itching in the affected area
- Imiquimod (Zyclara, Aldara) – Cream available with prescriptions only, enhances immune system’s ability to fight the virus. The cream might cause itching and pain on the site of application
Besides medications, other treatments for HPV include procedures[13] such as:
- Cryotherapy – Liquid nitrogen is used to burn abnormal cells
- Conization – Or cone biopsy, removes the abnormal areas
- Laser Therapy – Uses light to burn off abnormal cells
- Loop Electrosurgical Excision Procedure (LEEP) – Electrical current is used to remove abnormal cells
How to Prevent HPV Infection?
The human papillomavirus is widespread and, as stated above, most sexually active persons can get it. Although there is no sure way to prevent HPV, there are different things you can do to minimize your risk of getting infected. Below, you can see a list of useful strategies:
Abstinence
The only 100% effective way to prevent HPV is to abstain from sexual intercourse. Of course, this includes every kind of sexual intercourse, not just vaginal and anal, but oral too.
That being said, for most adults it’s impossible to practice abstinence completely, so you’ll still have to take other strategies into consideration.
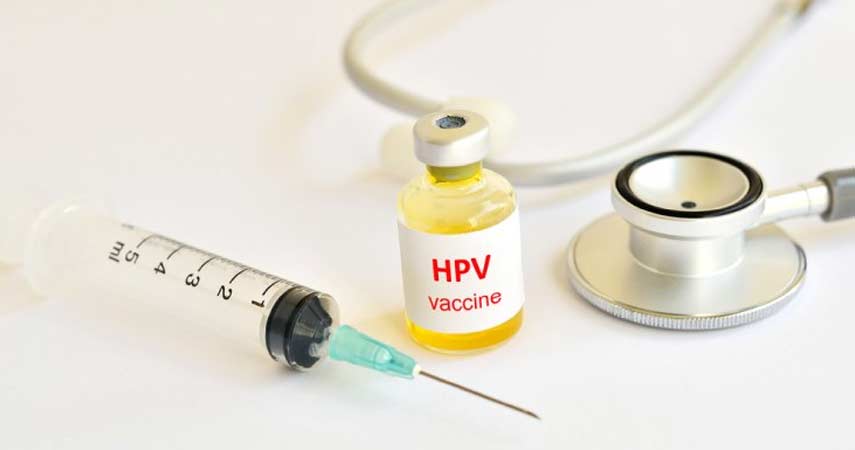
Vaccination
The FDA has approved two vaccines, Gardasil and Cervarix, to protect women against HPV types that cause cervical cancer. Plus, Gardasil protects women from uncomfortable and unsightly genital warts.
The vaccine is recommended for women ages 9 to 26, but older women can get it too. Gardasil protects men from genital warts too and it is, also, recommended for the 9-26 age group.
Avoid Having Multiple Sex Partners
The more sexual partners you have, the greater the odds of getting infected with HPV. In order to minimize the risk of getting the virus and experiencing an infection, it’s important to avoid having sexual intercourse with multiple partners.
Monogamous and committed relationships could help you cut down the risk, but it’s also recommended[14] one should know a partner for eight months or longer prior to deciding to have sexual intercourse with them. Why? That’s enough time for infection to clear out.
Condom Use

Practice safe sex in order to decrease the risk of getting the virus. That’s why men shouldn’t avoid using condoms as they provide a certain level of protection.
Bear in mind that condoms can’t protect you entirely, so you shouldn’t rely only on them. It’s important to use condoms from start to finish every sex act, including anal sex.
Circumcision
Circumcised men have a lower risk of both getting HPV and infecting their female sexual partners. If you’re not circumcised, consider getting it done.
Get Pap Test
Women should go to regular check-ups and consider getting a Pap test in order to find out whether they are infected or not. No need to wait until warts are formed.
Read More: Does Anal Sex Lead to HPV?
Outlook
Human papillomavirus is common and most people don’t know they have it until they notice warts or get diagnosed with cancer (in some cases). Bear in mind that having HPV, even high-risk type doesn’t indicate you’ll get cancer for sure.
Sometimes patients don’t even need medications, but in other instances they do. It’s important to see your doctor regularly, adhere to their recommendations, and practice safe sex.
Feature Image: Shutterstock.com
In-Post Image: Shutterstock.com & dawnsbrain.com








 This article changed my life!
This article changed my life! This article was informative.
This article was informative. I have a medical question.
I have a medical question.
 This article contains incorrect information.
This article contains incorrect information. This article doesn’t have the information I’m looking for.
This article doesn’t have the information I’m looking for.